Why Medicaid workflows struggle with document complexity and how AI standardizes review

TL;DR: Medicaid teams spend too much time deciphering inconsistent member documents instead of moving cases forward. Document intelligence uses AI and human validation to standardize reviews, surface integrity signals and produce audit-ready outputs, so eligibility and renewal workflows can scale with confidence.
Medicaid operations teams face a daily battle that has little to do with policy or funding. It has everything to do with paperwork. Eligibility determinations, renewals and verifications are document-heavy by design. The friction shows up when submissions arrive inconsistent, incomplete or hard to interpret.
That variability is not a minor inconvenience. It is a driver of backlogs, rework and inconsistent outcomes. When teams cannot quickly normalize what they are reviewing, they spend time rekeying data, chasing missing pages and reconciling conflicts across systems instead of making timely, defensible decisions.
The fastest path to scalable Medicaid document processing is not simply adding more staff to handle the volume. It is standardizing the document layer so every case starts from consistent, decision-grade information.
What makes Medicaid documents uniquely complex
Medicaid document workflows collide with scale and variance in ways most horizontal LLMs and automation tools underestimate.
Start with intake quality. Submissions range from clean PDFs to blurry smartphone photos, partial statements and handwritten annotations. A single upload can include multiple document types that require different handling.
Then add the breadth of documents. Depending on the population and program pathway, caseworkers may review income records, bank statements, benefit letters, residency documentation and tax forms. Requirements also diverge across MAGI and non-MAGI determinations, including aged, blind and disabled workflows and long-term care eligibility which often require deeper financial review.
Finally, many teams still manage fragmented systems for documentation, verification and review. Even with modernization initiatives, staff often must reconstruct a complete case narrative before they can decide what is missing, what conflicts and what can be verified.
Why compliance and program integrity raise the stakes
Medicaid decisions must be consistent, traceable and audit-ready. That standard becomes harder to meet when thousands of documents arrive daily in inconsistent formats. Federal requirements for renewals and redeterminations reinforce the need for structured verification and defensible processes, including rules outlined in 42 CFR part 435, subpart J.
When documents are processed inconsistently, downstream effects multiply. Corrections pile up. Appeals increase. Audit follow-ups consume staff time long after a case is closed. Program integrity pressure also rises at the document layer when submissions are incomplete, altered or contain conflicting information that is not flagged during initial review.
Why digitization alone fails in Medicaid workflows
Many agencies have already digitized documents. That is necessary, but it is not sufficient.
Basic OCR turns images into text. It does not create decision-grade evidence. Rules-only automation breaks when documents do not match expected templates. Neither approach reliably delivers normalized outputs, validation signals or explainable review artifacts that help staff make consistent decisions at scale.
This is where document intelligence differs from basic digitization. Ocrolus is an AI-powered workflow and data analytics platform that transforms messy documents and digital data into regulatory-grade decision intelligence. It blends best-in-class, domain-specific AI with human-in-the-loop validation so outputs are explainable and suitable for regulated workflows.
Medicaid workflows highlight a broader truth about regulated programs. Generic automation and large language models are not designed to deliver consistent, defensible outcomes at scale. In regulated environments, purpose-built AI that prioritizes control, consistency and traceable evidence is essential. For a deeper explanation of why this distinction matters, check out our recent blog: Purpose-built AI for regulated lending: where SLMs fit and why it matters
How AI standardizes review, step by step
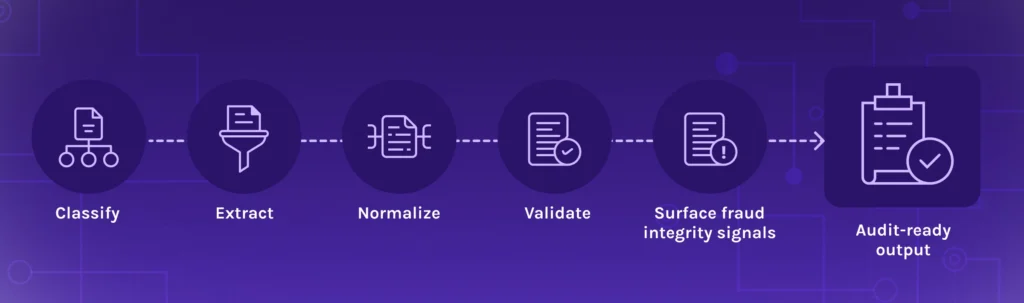
AI-driven workflows standardize Medicaid review by turning variable inputs into consistent, reviewable outputs. Together, these steps reduce rework, speed redeterminations and help eligibility staff focus on exceptions rather than rekeying data.
- Ingest and classify common eligibility and financial documents, even when formats vary
- Extract and normalize key data into consistent structures aligned to program requirements
- Validate and reconcile to surface missing items, mismatches and anomalies
- Surface integrity signals that help prioritize human review where it matters most
- Produce explainable outputs that support audit readiness and defensible decisioning
Ocrolus-reported metrics show it processes high volumes of documents and has delivered 50% to 75% reductions in document review time across applicable workflows. Results vary by program design, document quality and operational processes.
How it complements AVS and digital verification
Electronic verification systems can reduce manual collection in applicable cases. For individuals subject to an asset test, CMS guidance describes the role of asset verification systems in verifying assets held in financial institutions.
Digital sources complement, but do not replace, document-based verification in many workflows, especially when electronic sources are incomplete or not applicable. Document intelligence closes the gap by standardizing what members submit so caseworkers can resolve verification needs faster with a clearer evidence trail.
What to look for in Medicaid document intelligence solutions
When evaluating solutions, focus less on model branding and more on operational outcomes. Look for platforms that:
- Handle messy submissions at scale without requiring perfect inputs
- Produce explainable, audit-ready outputs that support compliance review
- Surface integrity signals, not just extracted fields
- Integrate with existing workflows and systems, including AVS where applicable
- Support multiple program pathways and state-specific variation
For broader guidance on evaluating AI in regulated workflows, explore the Ocrolus AI resource center.

Key takeaways
- Medicaid eligibility and renewals slow down when document variability drives rework and follow-ups
- Compliance and program integrity requirements make standardization essential
- OCR and rules-only automation do not produce decision-grade evidence on their own
- Document intelligence standardizes extraction, validation and review with humans in control
- AVS and electronic sources help, but documents still close gaps in many cases


